
Most people assume the challenges of aging are primarily medical. Research across multiple fields tells a more complete story.
A growing body of evidence — from the NIH, MIT, UCSF, Stanford, the Federal Trade Commission, and the U.S. Senate Special Committee on Aging — documents that life complexity grows substantially in later life across many dimensions that have little to do with clinical health. Technology has reorganized daily life around digital systems built for younger users. A lifetime of living fills a home with possessions that become harder to manage precisely when the executive function needed to address them is in gradual decline. Retirement simultaneously triggers peak asset complexity and peak vulnerability to financial exploitation. The informal network of spouses, siblings, and lifelong friends — the people who shared the cognitive load of living — quietly diminishes.
Life Complexity Keeps Increasing As Our Ability to Deal with this Complexity Diminishes
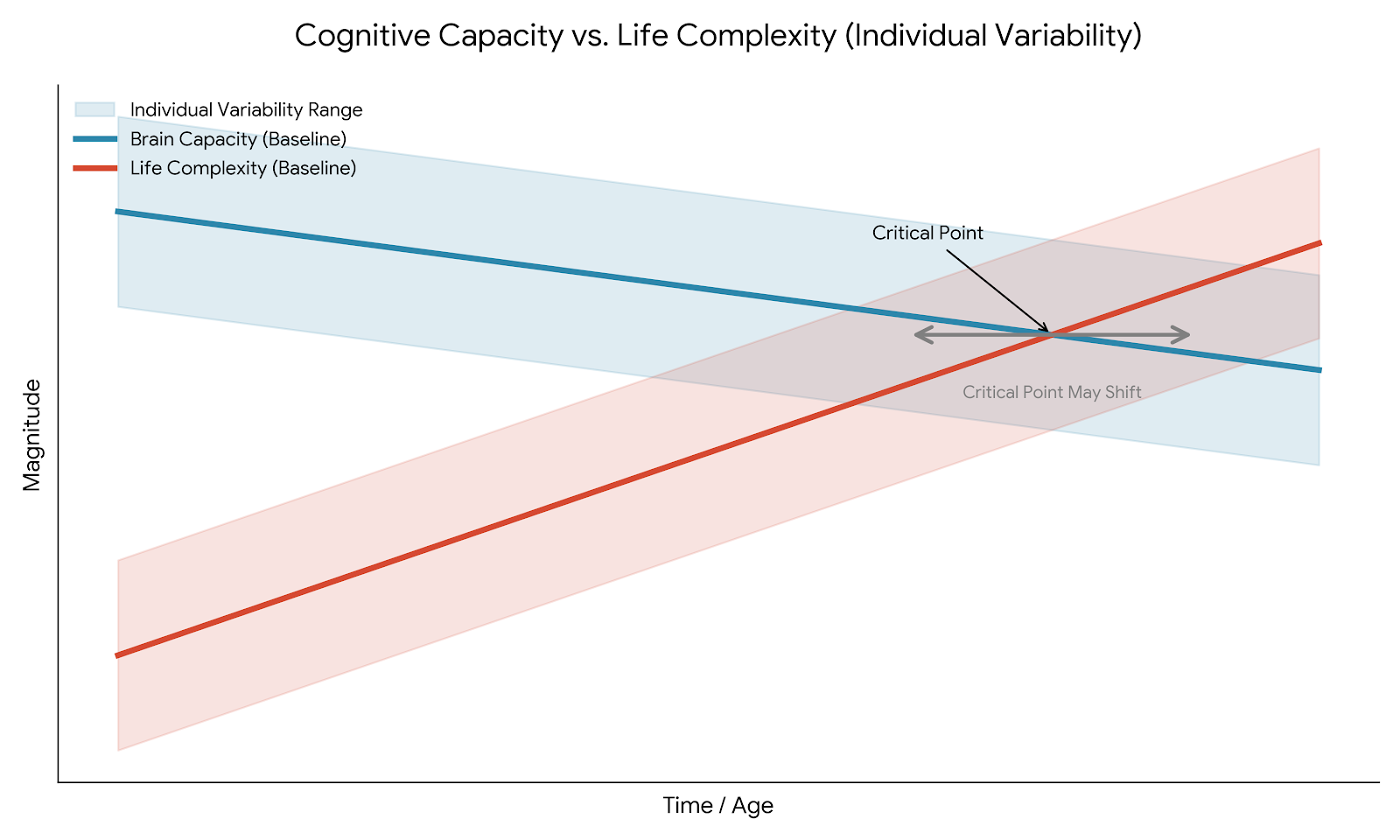
The Life Operating System maps these evidence-based complexity drivers to its Four Pillars: Daily Life & Identity, Health & Care Infrastructure, Authority & Protection, Decisions & Coordination. The framework below is an original synthesis by Peritus & Company, drawing on research across gerontology, neuroscience, public health, behavioral economics, and elder law. Each of the eight domains is individually supported by peer-reviewed and government research. The critical insight is not that these challenges exist — it's that they converge, compound, and arrive precisely when cognitive capacity for managing them is most stretched.
as We Get Older